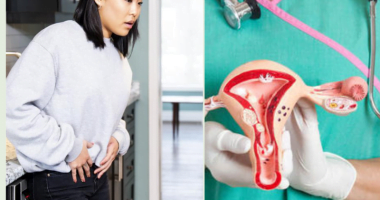
Among diabetic pregnant women, the most common problem when it comes to their baby’s health is the condition called “macrosomia” or having a baby with large body.
This is because during pregnancy the blood of the mother with diabetes is interchanged with that of the baby inside the womb. As a result, the baby will produce insulin to be able to glucose and this will lead to fat deposits, which causes the baby to grow larger than the regular size of newborns
One research reported that nearly 10% of all pregnancies are affected by macrosomia.
Another research showed that about 15 – 45% of newborns of women with gestational diabetes are larger than the regular baby size while only 12% newborns of normal women are affected with macrosomia.
What causes this condition?
The size of your baby is most likely to be affected when;
- You have gestational diabetes( diabetes during pregnancy)
- You have got diabetes before pregnancy
- You have obesity in your blood history (genetics)
- Your baby has been diagnosed with a medical condition.
- You gain excessive weight during pregnancy
- Your maternal age is over 35 years
- You have high blood pressure during pregnancy
- You previously had a baby with macrosomia
Maternal Complications of Macrosomia
If the baby is typically large, the following problems may arise in the course of delivery:
- The labor duration may take longer than normal.
- The fetus’s shoulder may get stuck in the birth canal.
- The baby’s clavicle or another bone may get fractured.
- Laceration and tear of the vaginal tissue may be necessary.
- Instrumental delivery (with forceps or vacuum) may be needed.
- An unplanned or emergency cesarean section may be necessary.
- The baby’s accessibility of oxygen may be limited.
- Excessive bleeding after delivery may occur.
- The mother may have genital tract Injury.
- The mother may have uterus tear especially if she has had cesarean delivery in the past.
Fetus Complications of Macrosomia
Premature Birth. Due to the early induction of labor before 39 weeks of gestation and/or premature rupture of membranes, there is a risk of preterm delivery.
Although all the necessary precautions are undertaken prior to the induction of early labor, newborns are still under the risk of complications associated with prematurity, including difficulties in respiration and feeding, infection, jaundice, neonatal intensive care unit admission and perinatal death.
Shoulder Dystocia and Erb’s Palsy. One of the most serious complications of vaginal delivery in macrosomic babies is shoulder dystocia which is associated with birth trauma. Newborns with a birth weight of 4,500 g or more carry a 6 times higher risk of birth trauma.
Hypoglycemia at Birth. This occurs due to the hyperinsulinemia of the fetus in response to the maternal hyperglycemia in utero. It can lead to more serious complications like mental retardation, recurrent seizure activity, developmental delay and personality disorders.
Neonatal Jaundice. Factors that may account for jaundice are prematurity, impaired hepatic conjugation of bilirubin and increased enterohepatic circulation of bilirubin resulting from poor feeding.
In macrosomia, neonates have a high oxygen demand causing increased erythropoiesis and, ultimately, polycythemia. Therefore, when these cells break down, bilirubin (a byproduct of red blood cells) increases resulting in neonatal jaundice.
Congenital Anomalies. Heart defects and neural tube defects, such as spina bifida, are the most common types of birth defects. The high blood sugar level of women with Gestational diabetes can damage the developing organs of the fetus, leading to congenital anomalies.
More Complications that may occur later in the life of the baby.
Offspring of diabetic mothers is also susceptible to the onset of metabolic syndromes such as:
- Obesity
- Higher Body Max Index (BMI)
- Abnormal cholesterol levels
- Heart disease,
- Stroke
- Diabetes.
Medical preventive measure
Experts have suggested that the complications during delivery caused by macrosomia can be prevented by delivery via elective cesarean. This strategy should only be considered when the estimated fetal weight is over 4500 g or over 5000 g in women without diabetes
Another strategy to overcome the negative impacts of macrosomia is early induction of labor to reduce the likelihood of fetal growth; however, the increased risks of maternal and neonatal morbidity and mortality associated with induction should be taken into consideration
Natural Preventive measures
For a healthy lifestyle during pregnancy, it is ideal to maintain an appropriate weight gain, the average consumption of various foods from different food groups, timely and prescribed vitamin and mineral supplementation, and lots of fluid intake.
Sweets and fats should also be kept to a minimum level of consumption. The following are just some of the guidelines that pregnant women with diabetes can use to achieve healthy pregnancy despite the chronic disease:
1. Follow the appropriate meal plan religiously. More than ever, pregnant women should pay attention to what they eat and their eating patterns in general. This is very important because this stage—pregnancy itself—requires strict control of blood glucose levels in order to ensure that both the mother and baby are getting the right amount of key nutrients needed.
In coming up with the right diet plan, it is best to seek the help of a diabetes educator or a licensed dietitian. Necessary adjustments needed to accommodate the needs of the fetus inside the womb and the mother as well.
In your meal plan, take note of calorie, carbohydrates and protein requirements every day because these will help you maintain normal blood glucose levels.
2. Regular Self-Monitoring of Blood Glucose or SMBG. Experts say that the only way to tell if the woman is successful in controlling her blood glucose is to monitor their levels by themselves regularly.
Since being pregnant is a sensitive condition, soon to be mothers should monitor their blood glucose levels more frequently. Ideally, SMBG should be monitored four to 10 times a day.
3. Knowledge on how to administer insulin injections. A sufficient supply of insulin is very crucial for pregnant women so they must know how to administer insulin injections by themselves in case no one is around when they need it.
They should also ask their physicians how to adjust the doses of insulin after they are through with the SBMG. Knowing how to adjust the doses of insulin needed is very important to ensure that the body’s supply of insulin is stable.
4. Treating or controlling hypoglycemia. Pregnant women who are diabetics are more prone to hypoglycemia because of the hormonal changes in their body.
Although studies show that there are no known effects of hypoglycemia in the baby, it is best to control or treat it as soon as possible so the soon to be mom won’t be having troubles during the course of conception.
5. Maintaining a regular set of exercise or physical activities. This is also very important for pregnant women with diabetes because through this they can reduce the risk of hypoglycemia as well as being overweight.
Since it is hard for pregnant women to do strenuous workouts, it is best to maintain the hobby of having light exercises that will keep the body moving.
SHOP HEALTH PRODUCTS @ AMAZING LOW PRICES
POST SOURCE Sound Health and Lasting Wealth